A Comprehensive Guide to Finger Selection for Optimal Oxygen Saturation Monitoring
Introduction
Why Finger Selection Matters in Accurate SpO₂ Readings
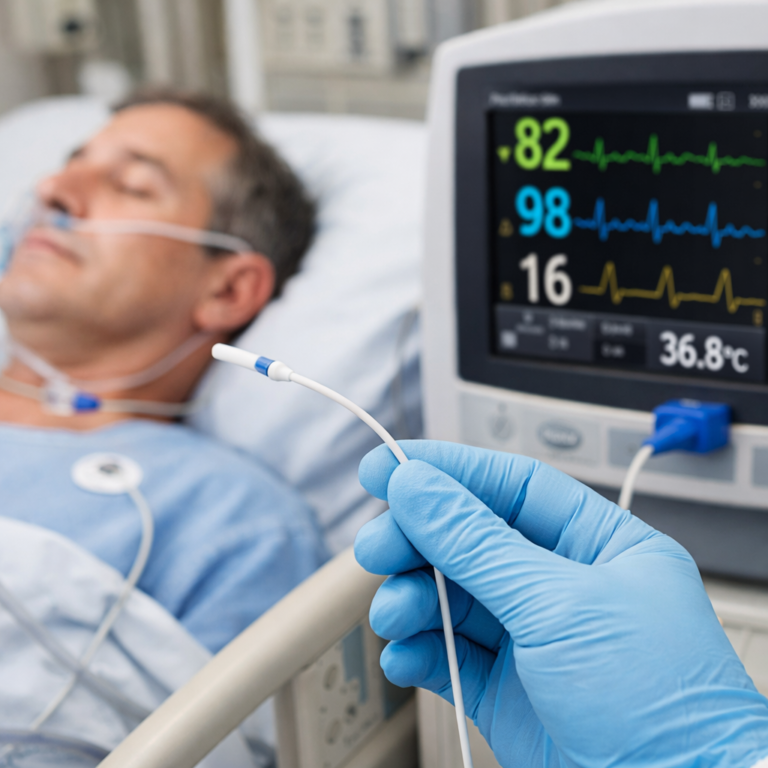
SpO₂ monitoring is a frontline diagnostic measure in both acute and chronic care settings. However, the accuracy of these readings can be influenced by a surprisingly nuanced variable—finger selection. While the technology behind pulse oximetry is sophisticated, the choice of digit plays a pivotal role in ensuring signal integrity and reliable data. Choosing the optimal finger enhances clinical decision-making and reduces false alarms or erroneous interventions.
The Overlooked Variable in Patient Monitoring: Finger Choice
Amidst the rush of critical care, clinicians often prioritize convenience or habit over precision when applying pulse oximeter sensors. Yet finger anatomy, perfusion variability, and physiological conditions can all distort results if the site is suboptimal. Recognizing finger choice as a controllable factor is essential for elevating the reliability of patient monitoring.
The Ideal Finger for SpO₂ Monitoring
Why the Index Finger Is Commonly Preferred
The index finger reigns as the default choice in most clinical environments. Its robust arterial supply and straightforward alignment with most clip-type sensors provide dependable optical transmission. Additionally, it’s less prone to involuntary movement than the thumb, making it ideal for both resting and conscious patients. Many oximeters are factory-calibrated with the index finger in mind, reinforcing its place as the gold standard.
Advantages of the Middle Finger in Sensor Placement
The middle finger, with its slightly larger diameter and central alignment in the hand, offers consistent capillary perfusion. This makes it an excellent alternative when the index is unavailable. Its positioning also benefits from reduced motion interference, particularly in patients who are sedated or immobilized. The bone structure and soft tissue distribution in the middle finger often accommodate snug sensor fitment, preserving signal quality.
Ring Finger Readings: When and Why They Work
Although not a first-line choice, the ring finger can serve reliably when other digits are compromised. In some patients, particularly those with vascular disease or peripheral edema, the ring finger shows better perfusion than expected. This finger may also be preferable in post-surgical cases involving the radial side of the hand or when other sites are inaccessible.
Little Finger Considerations: Pros and Limitations
The little finger, or fifth digit, presents a mixed bag. On the one hand, its small size allows rapid placement and reduced sensor slippage in pediatric or petite adult patients. On the other hand, perfusion is frequently weaker, and the digit is more prone to thermal fluctuations, resulting in erratic readings. It should be considered only when better sites are unavailable or in specialized use cases.
The Thumb Debate: Anatomical Challenges and Signal Quality
The thumb offers a robust blood supply but comes with several caveats. Its muscular structure and increased movement frequency pose risks for signal artifacts. Additionally, its broader surface area can distort LED and photodetector alignment. Though usable in emergencies, the thumb generally lacks the consistency required for dependable SpO₂ monitoring.
Physiological Factors That Affect Finger Selection
Blood Perfusion and Its Influence on Reading Accuracy
Optimal SpO₂ readings rely on healthy blood flow through peripheral capillaries. Fingers with compromised perfusion—due to cold, hypotension, or vascular conditions—can mislead the monitor. Selecting the finger with the strongest pulse, often determined by touch or visual inspection, increases the chances of acquiring a reliable waveform.
Temperature and Vasoconstriction: How Cold Fingers Skew Results
Hypothermia or ambient cold can induce peripheral vasoconstriction, dramatically reducing blood flow to the fingers. This reduction impairs light absorption and disrupts waveform stability. In such instances, warming the hand or switching to a better-perfused finger or alternative site becomes essential.
Nail Polish, Artificial Nails, and Their Impact on Light Transmission
Colored nail polish, especially darker shades like black or navy blue, can block the red and infrared light used in pulse oximetry. Acrylic or gel nails further obstruct the photodetector’s ability to measure oxygen saturation. If removal is impractical, choosing a finger without such obstructions—or using side placement techniques—can mitigate interference.
Skin Thickness and Tissue Density: Do They Matter?
Yes, they do. Excessive callousing, scarring, or edema can affect the optical pathway. Fingers with uniform, thinner skin provide clearer signal transmission. Evaluating skin integrity before sensor placement is a subtle but impactful step in enhancing measurement fidelity.
Hand Dominance and SpO₂ Accuracy
Dominant vs. Non-Dominant Hand: Does It Influence Readings?
Studies suggest that the non-dominant hand may exhibit slightly better perfusion due to reduced muscular engagement. While the difference is often marginal, clinicians may favor the non-dominant hand when readings from the dominant side show anomalies. This tactic can be particularly useful in long-term monitoring where muscular contractions influence results.
Muscle Tone, Movement, and Signal Stability
Muscle contractions—conscious or reflexive—can cause micro-movements that disrupt the sensor’s alignment. This results in erratic signals or loss of data. Fingers with less voluntary movement, especially in sedated or resting patients, tend to provide cleaner, uninterrupted waveforms.
When the Preferred Fingers Are Not Available
Alternatives for Patients with Trauma, Amputations, or IV Lines
In trauma patients or those with IV lines, burns, or bandaging, conventional finger options may be compromised. In such cases, clinicians must pivot to less traditional sites, ensuring sensor compatibility and signal quality through careful placement.
Using Toes, Ears, or Forehead Sensors as Backups
Toes offer a practical alternative, especially in bedridden patients. Earlobes, with consistent perfusion and minimal movement, are another dependable site. Forehead sensors—using reflectance technology—are increasingly employed in critical care, particularly during surgeries or transport scenarios where extremities are inaccessible.
Pediatric and Neonatal Considerations in Site Selection
Infants and neonates present unique challenges due to their diminutive anatomy and fragile skin. Wrap-around sensors on the foot or palm are commonly used. The finger may be too small or too active to maintain sensor stability, making alternative sites more viable. Special pediatric sensors are designed with soft adhesives and flexible materials for gentle application.
Clinical Guidelines and Best Practices
What Studies Say About Finger Preference and Reliability
Peer-reviewed research underscores the importance of finger selection. The index and middle fingers consistently outperform other digits in signal stability and waveform clarity. These findings guide clinical protocols, especially in high-dependency units where accuracy is paramount.
Recommendations from Monitoring Device Manufacturers
Leading pulse oximeter manufacturers such as Masimo, Nellcor, and Mindray often recommend the index or middle finger for standard use. Their devices are calibrated based on controlled testing at these sites, making adherence to these recommendations vital for expected performance.
Hospital Protocols and Standard Operating Procedures
Many healthcare institutions outline preferred monitoring sites in their standard operating procedures. These guidelines not only optimize efficiency but also ensure consistency across clinical staff. Regular training and updates reinforce the importance of selecting the right finger based on the patient’s condition and device used.
Discover Medke’s SpO₂ Sensors Designed for Every Finger and Clinical Need
Medke offers a wide spectrum of SpO₂ sensors tailored to various anatomical sites and patient populations. From adult clip sensors to soft neonatal wraps, our products deliver precision, comfort, and compatibility across all major patient monitors.
Our clinical product advisors are ready to help you select the most appropriate sensor for any scenario. Whether you’re navigating complex ICU protocols or outfitting your clinic with dependable monitoring tools, we provide the expertise to support your needs with confidence and clarity.
11.png)