A Comprehensive Guide to Oxygen Saturation and Its Clinical Importance
Introduction
The Lifeline of Oxygen: Understanding SpO₂ in Modern Medicine
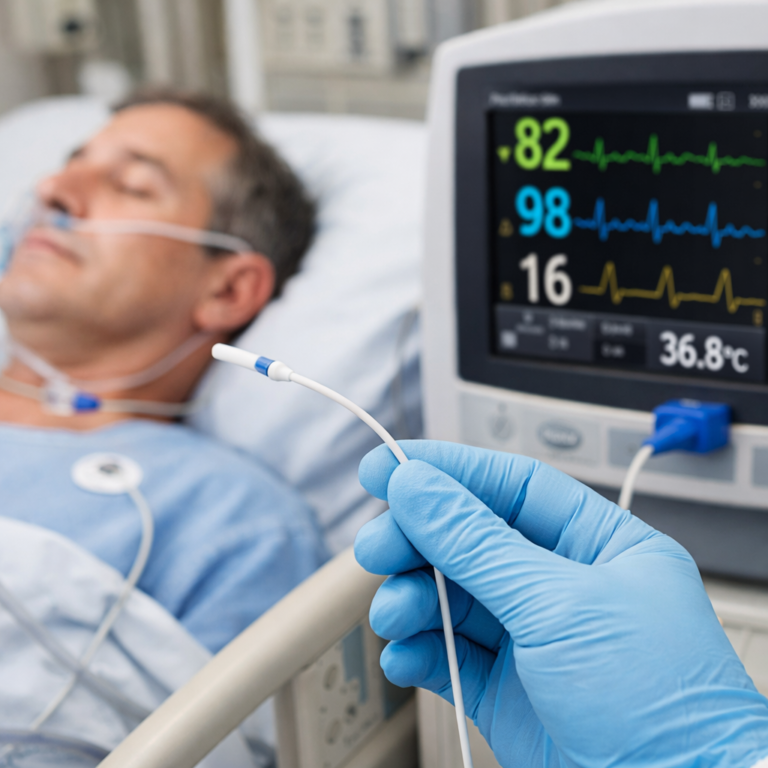
Oxygen is fundamental to sustaining life, fueling every cellular function from brain activity to muscular contraction. When oxygen levels fall below normal, cells begin to fail, organs suffer, and systems start to deteriorate. SpO₂—or peripheral capillary oxygen saturation—acts as a non-invasive window into the body’s ability to transport and deliver this vital gas. In modern medicine, where timely intervention can determine survival, tracking oxygen saturation is indispensable.
Why SpO₂ Is One of the Five Essential Vital Signs
Alongside temperature, heart rate, blood pressure, and respiratory rate, SpO₂ has been universally adopted as a fifth vital sign. Its inclusion reflects its diagnostic utility across nearly every medical discipline. A single drop in oxygen saturation can flag early signs of respiratory compromise, cardiac failure, or circulatory collapse. Clinicians rely on this data to make real-time decisions that affect triage, treatment, and prognosis.
Understanding the Basics of SpO₂
What Does SpO₂ Stand For?
SpO₂ stands for peripheral capillary oxygen saturation. It represents the percentage of hemoglobin in the blood that is saturated with oxygen. Derived from “Saturation of Peripheral O₂,” this value provides a snapshot of how efficiently the lungs are oxygenating blood and how well the cardiovascular system is distributing it to tissues.
How SpO₂ Reflects Blood Oxygenation Status
As oxygen enters the lungs and diffuses into the bloodstream, it binds to hemoglobin molecules within red blood cells. SpO₂ measurement reflects the proportion of these hemoglobin molecules that are carrying oxygen. A reading of 98%, for example, means that 98 out of every 100 hemoglobin units are oxygen-saturated—a direct indicator of respiratory and circulatory efficiency.
The Difference Between SpO₂ and SaO₂: A Clarification of Terms
While often used interchangeably, SpO₂ and SaO₂ differ in method and specificity. SpO₂ is estimated non-invasively using a pulse oximeter, while SaO₂ (arterial oxygen saturation) is measured directly from arterial blood through a blood gas analysis. Though their values typically align, SaO₂ offers greater accuracy in complex clinical cases. SpO₂ remains the more convenient, real-time indicator used in routine and emergency care.
Normal SpO₂ Ranges Across Age Groups and Health Conditions
In healthy individuals, normal SpO₂ values generally range between 95% and 100%. Slight deviations may occur in older adults or individuals with chronic respiratory conditions, where readings in the 90–94% range might be considered baseline. Persistent values below 90%—termed hypoxemia—require immediate evaluation and often supplemental oxygen or ventilatory support.
How SpO₂ Is Measured
The Science Behind Pulse Oximetry
Pulse oximetry is the method by which SpO₂ is determined, using light-based technology to measure the ratio of oxygenated to deoxygenated hemoglobin. A sensor is placed on a thin part of the body, typically a fingertip or earlobe, where light can pass through capillary-rich tissue. The device interprets light absorption patterns to compute oxygen saturation.
Wavelengths and Light Absorption: Red vs. Infrared Technology
Pulse oximeters use two specific light wavelengths—red (approximately 660 nm) and infrared (approximately 940 nm). Oxygenated hemoglobin absorbs more infrared light, while deoxygenated hemoglobin absorbs more red light. By comparing how much light at each wavelength passes through the tissue, the device calculates the saturation percentage with remarkable speed and accuracy.
How Sensors Detect Pulsatile Arterial Flow
A key aspect of pulse oximetry is its ability to detect pulsatile changes in blood volume caused by each heartbeat. This pulsation allows the device to isolate arterial blood from the static presence of venous blood and surrounding tissue. The resulting photoplethysmographic signal is filtered and digitized to ensure that only dynamic, oxygen-rich arterial flow contributes to the final reading.
Common Anatomical Sites for SpO₂ Monitoring
The most frequently used sites for SpO₂ measurement include the fingertip, earlobe, and toe. In neonatal care, the palm or foot may be used. Forehead sensors are also employed during surgery or in cases of poor peripheral perfusion. Each site has specific advantages and is chosen based on the patient’s condition, mobility, and environmental context.
Clinical Importance of Monitoring SpO₂
Early Detection of Hypoxemia in Acute Settings
A sudden drop in SpO₂ can be the first indication of a life-threatening event. In emergency rooms and trauma settings, pulse oximetry allows clinicians to assess oxygenation within seconds. Early hypoxemia detection leads to faster airway management, oxygen therapy, or escalation to mechanical ventilation.
Monitoring Respiratory Conditions: COPD, Asthma, and Pneumonia
In chronic and acute respiratory conditions, SpO₂ monitoring provides insight into the severity of airway obstruction, infection, or gas exchange impairment. For patients with COPD or asthma, staying within a target saturation range is critical to avoiding exacerbations. In pneumonia, SpO₂ helps assess treatment efficacy and the need for hospitalization.
SpO₂ Tracking in Post-Surgical Recovery and Anesthesia
Anesthesia can depress respiratory drive and reduce oxygenation. Continuous SpO₂ monitoring during surgery ensures the patient remains within safe oxygen thresholds. Postoperatively, it guards against hypoventilation caused by sedatives, opioid analgesics, or residual anesthetic agents.
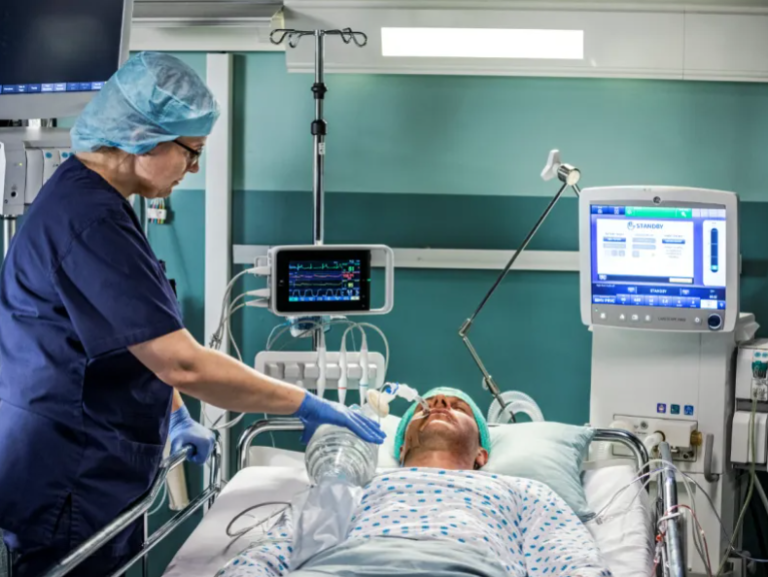
Oxygen Saturation Monitoring in Critical Care and ICU
In ICUs, SpO₂ is monitored continuously alongside heart rate and blood pressure. It assists in ventilator titration, weaning protocols, and the early identification of septic shock or cardiac deterioration. Maintaining optimal oxygen levels is central to organ preservation and overall survival.
Remote Monitoring in Homecare and Telemedicine
The expansion of telehealth has brought SpO₂ monitoring into the home. Patients with heart failure, COVID-19, or chronic lung disease can be remotely tracked through wearable pulse oximeters. Clinicians receive real-time alerts if saturation drops, enabling timely intervention without hospitalization.
Conclusion
Though small in appearance, the SpO₂ percentage holds profound clinical weight. It encapsulates the body’s oxygen supply chain—from lung function to tissue delivery—in a single, accessible value. Its continuous measurement has revolutionized how healthcare providers monitor, diagnose, and respond to patient needs.
Emerging innovations in pulse oximetry promise enhanced accuracy, miniaturization, and integration with AI-driven platforms. Future sensors may not only measure saturation but also predict deterioration before it occurs. As healthcare embraces precision medicine, SpO₂ will remain a cornerstone—quietly guiding the way toward safer, smarter, and more responsive care.
11.png)