A Comprehensive Guide to Resolving Common Problems in Pulse Oximetry
Understanding Normal vs. Abnormal Sensor Behavior
Recognizing Valid SpO₂ Readings vs. Erratic or Flat-Line Values
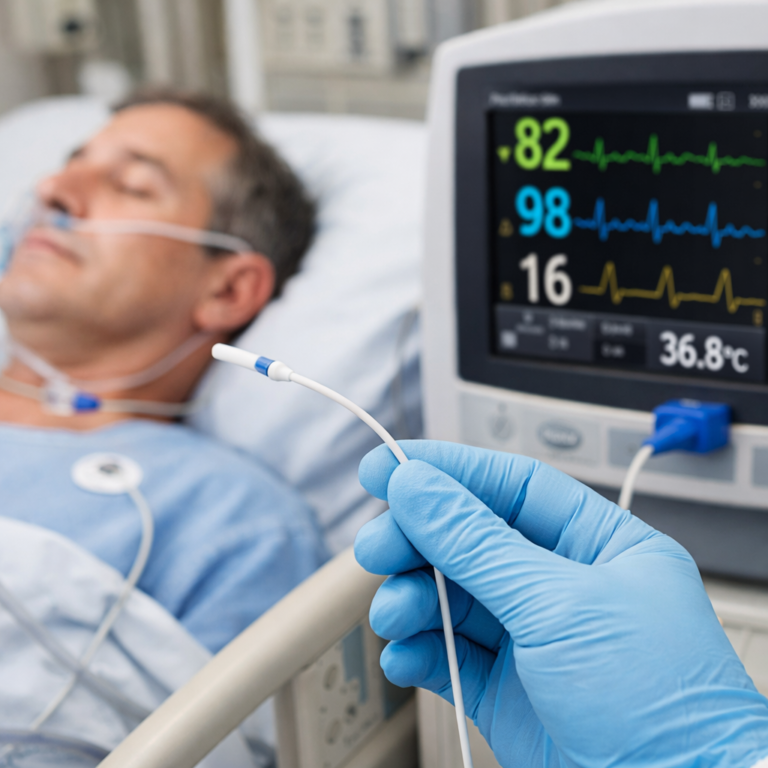
A properly functioning SpO₂ sensor should produce a stable, physiologically consistent reading—typically between 95–100% in healthy individuals. Any sudden, unexplained drop in saturation, especially in the absence of respiratory or circulatory distress, should prompt suspicion. Flat-line values (such as a frozen display or zero reading) are rarely true reflections of patient status and more often symptomatic of technical issues or poor sensor contact.
What a Healthy Pleth Waveform Should Look Like
The plethysmographic waveform displayed alongside the SpO₂ value is a crucial diagnostic ally. A healthy pleth waveform should be regular, rhythmic, and reflective of the patient’s pulse. It should display a consistent amplitude and shape. Irregular peaks, low amplitude, or completely absent waveforms suggest motion artifacts, low perfusion, or faulty sensor placement—each requiring immediate attention.
Common Symptoms of Sensor Malfunction
Intermittent Signal Dropouts or SpO₂ Fluctuations
Frequent signal loss or wildly fluctuating readings—especially if not correlated with clinical symptoms—are red flags. These may be caused by sensor movement, loose connections, or interference. Consistency is key in pulse oximetry; unstable outputs undermine clinical reliability.
Low or Inaccurate Saturation Readings in Otherwise Stable Patients
If a patient presents no signs of distress—normal respiratory rate, pink skin, stable heart rate—but the SpO₂ reading is unexpectedly low, technical issues should be considered. Sensor misalignment, ambient light interference, or optical contamination may be the culprit.
“No Sensor Detected” or “Check Probe” Monitor Alerts
When the monitor fails to recognize the sensor, it often indicates a disconnected or damaged probe, incompatible device pairing, or internal malfunction. Such alerts should never be dismissed—they signal either hardware failure or improper setup.
Delayed or Frozen Waveform Display
If the pleth waveform appears stuck or slow to respond to physiological changes, there may be lag in signal processing or degraded sensor optics. This delay in feedback compromises real-time monitoring and must be resolved swiftly.
Mechanical and Placement Issues
Improper Sensor Positioning on the Finger, Toe, or Alternate Sites
Correct placement ensures optimal light transmission through pulsatile vascular tissue. Mispositioned sensors may fail to detect pulses or misread oxygen saturation. The emitter and detector must be aligned across the nail bed or thin tissue for accuracy.
Sensor Slippage During Movement or Restless States
Even minor shifts in sensor placement during movement can disrupt readings. Children, uncooperative patients, or those experiencing tremors are especially vulnerable to this issue. Using adhesive-secured sensors or wraps can help stabilize the probe.
Cable Bending, Twisting, or Pinching Affecting Signal Integrity
Cables are often the weakest link. Repeated bending or pinching can cause internal wire fractures or signal dropouts. Careful cable management—avoiding sharp angles and entrapment—is essential for sustained sensor performance.
Patient-Related Factors Affecting SpO₂ Readings
Poor Perfusion: Cold Extremities, Shock, or Vasoconstriction
Low peripheral perfusion limits the pulsatile signal needed for accurate SpO₂ detection. Hypothermia, hypovolemia, or vasopressor use can all contribute to poor signal quality. Warming the extremity or selecting a better-perfused site (e.g., ear lobe or forehead) may restore reliable readings.
Dark Nail Polish, Artificial Nails, or Skin Pigmentation
Pigments in nail polish or melanin in the skin can absorb light wavelengths used in pulse oximetry, leading to falsely low readings. Removing polish, using alternative sites, or using sensors with adaptive algorithms can mitigate this issue.
Motion Artifacts from Shivering, Tremors, or Seizures
Motion can mimic or mask the true pulsatile signal. Advanced monitors with motion-tolerant algorithms help, but stabilization of the sensor and patient remains the first line of defense. In some cases, it may be necessary to pause monitoring until the motion subsides.
Excessive Ambient Light Interference in Bright Environments
Operating rooms, trauma bays, and sunlit recovery rooms often introduce intense ambient light, which competes with the sensor’s infrared and red light transmission. Shielding the sensor with a drape or using opaque covers can reduce this interference.
Sensor and Hardware Evaluation
Inspecting the Sensor for Physical Damage or Wear
Visual inspection can reveal a lot—cracked housings, dirty optical surfaces, or worn connectors are common culprits. Sensors that appear damaged should be retired and replaced immediately.
Verifying Secure Connection at the Monitor Port
Loose or partially connected probes can produce intermittent readings or system alerts. Ensuring a firm, secure connection with audible or tactile feedback helps avoid false signal dropouts.
Testing with a Replacement Sensor to Rule Out Device Issues
One of the fastest ways to isolate a faulty sensor is to swap it with a known working unit. If the issue resolves, the original sensor is likely defective. If the problem persists, the monitor or port may require further assessment.
Confirming Sensor Compatibility with the Patient Monitor Model
Using sensors that are not OEM-compatible can result in communication errors, inaccurate readings, or total non-functionality. Always confirm compatibility, especially when using third-party or reusable probes.
Environmental and Electrical Interference
Electromagnetic Interference from Nearby Equipment
Infusion pumps, defibrillators, MRI scanners, and other powered devices may emit electromagnetic fields that interfere with SpO₂ readings. Repositioning equipment or using shielded cables can minimize this risk.
Light Leakage from Surgical Lamps or Sunlight Exposure
Surgical and examination lights—particularly LED and halogen sources—emit wavelengths that overlap with those used in SpO₂ detection. Light shields or sensor wraps help isolate the signal.
Effects of High-Altitude or Low-Humidity Environments
At high altitudes, baseline SpO₂ values drop physiologically. However, low humidity can dry out adhesive-backed sensors, weakening contact and affecting signal. Site rotation and humidification of the sensor area can help maintain functionality.
Best Practices for Sensor Cleaning and Maintenance
Proper Disinfection Methods to Prevent Residue or Optical Obstruction
Residue from improper cleaning solutions can fog the optical window, degrading signal clarity. Only manufacturer-approved disinfectants should be used, and sensors should be dried completely before reuse.
Avoiding Harsh Chemicals that Degrade Sensor Housing or Lenses
Bleach, alcohol, or acetone can cause plastic or lens distortion over time. These materials may cloud optical paths or weaken casings, resulting in sensor failure. Non-corrosive, low-pH cleaners are preferred.
Guidelines for Reusable vs. Disposable Sensor Handling
Reusable sensors must be cleaned between patients without compromising their optical surfaces. Disposable sensors should be discarded after single use, especially if adhesive integrity or hygiene is compromised. Clear labeling and staff education help enforce proper usage protocols.
Conclusion
Proactive Troubleshooting as a Core Element of Patient Monitoring
Troubleshooting SpO₂ issues is not simply technical housekeeping—it is a clinical necessity. Every inaccurate reading or missed alert represents a lost opportunity for early intervention. By equipping staff with the knowledge and confidence to diagnose and resolve sensor issues, healthcare teams can maintain the highest standards of patient care.
The Importance of Training, Checklists, and Preventive Maintenance
Consistent training, usage checklists, and proactive equipment maintenance reduce sensor failures and improve overall system uptime. Investing in preventive strategies and staff competency ensures that SpO₂ sensors remain a dependable, accurate window into the patient’s oxygenation status—every time, without exception.
11.png)