A Comprehensive Insight into Multi-Parameter Monitoring in Modern Medicine
Introduction
The Power of Integration: Why Multi-Parameter Monitoring Matters
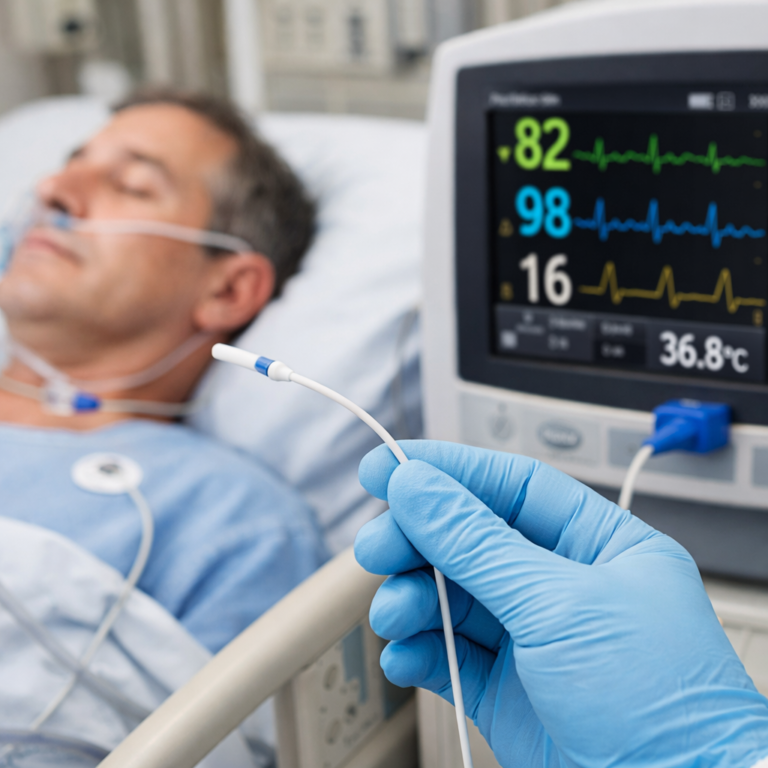
In today’s clinical landscape, isolated data points no longer suffice. High-acuity environments demand comprehensive, real-time insight into a patient’s physiological state. Multi-parameter monitoring—where SpO₂, ECG, NIBP, and temperature data are evaluated in tandem—enables clinicians to make swift, informed decisions. This synergistic approach helps decode the body’s complex signals before deterioration becomes visible.
Understanding the Interconnectedness of Vital Signs in Patient Care
The human body operates as an integrated system, where changes in one vital sign ripple across others. Oxygen saturation, cardiac rhythm, circulatory pressure, and thermal regulation are not isolated processes—they are tightly interwoven physiological expressions. Monitoring them together enhances diagnostic clarity, flags early warning signs, and supports more nuanced interventions.
Overview of Core Physiological Parameters
SpO₂, ECG, NIBP, and Temperature: What Each Measures and Why
- SpO₂ (Peripheral Oxygen Saturation): Indicates the percentage of hemoglobin saturated with oxygen—an essential measure of respiratory and circulatory efficiency.
- ECG (Electrocardiogram): Captures the electrical activity of the heart, revealing arrhythmias, ischemia, or conduction disturbances.
- NIBP (Non-Invasive Blood Pressure): Reflects the mechanical force of circulating blood against arterial walls, giving insight into perfusion status.
- Temperature: Serves as a proxy for metabolic demand, infection, inflammation, and thermoregulatory balance.
Together, these parameters form a physiological matrix that defines patient stability.
SpO₂ and ECG: Linking Oxygen Saturation with Cardiac Rhythm
How SpO₂ Trends Reflect Cardiac Output and Perfusion
Oxygen saturation relies on the circulatory system to deliver oxygen-rich blood. If cardiac output drops—due to bradycardia, tachycardia, or poor contractility—SpO₂ readings may decrease even if the lungs are functioning properly. Monitoring ECG alongside SpO₂ allows clinicians to assess whether desaturation is a pulmonary issue or a perfusion failure.
Using ECG to Interpret Arrhythmias That Affect Oxygen Delivery
Cardiac arrhythmias, such as atrial fibrillation or ventricular tachycardia, can significantly impair oxygen transport. Coupling ECG data with SpO₂ trends helps clinicians determine whether rhythm disturbances are compromising effective oxygen delivery—allowing for immediate rhythm correction or pharmacological support.
Synchronizing Pulse Oximetry and Heart Rate for Diagnostic Clarity
Pulse oximeters typically provide a plethysmographic waveform, which corresponds with heart rate. When ECG and SpO₂ heart rates are desynchronized, it may signal signal dropout, poor perfusion, or sensor misplacement. Real-time correlation validates the integrity of monitoring data and confirms accurate pulse detection.
SpO₂ and NIBP: Assessing Perfusion Under Pressure
The Relationship Between Blood Pressure and Oxygen Delivery
Adequate blood pressure is crucial for ensuring that oxygenated blood reaches peripheral tissues. Low NIBP values can render SpO₂ readings unreliable—not because the lungs aren’t oxygenating, but because insufficient perfusion prevents accurate detection. Monitoring both simultaneously bridges this diagnostic gap.
Hypotension and Hypoxia: Dual Red Flags in Critical Care
When hypotension coincides with low SpO₂, the patient may be in shock or experiencing acute cardiovascular collapse. Recognizing this pairing early is vital in initiating fluid resuscitation, vasopressors, or mechanical support. The tandem drop in these vitals often indicates a system-wide failure requiring immediate intervention.
High Blood Pressure and Vasoconstriction Effects on SpO₂ Readings
Conversely, elevated blood pressure may cause peripheral vasoconstriction, reducing the signal strength at the sensor site. While SpO₂ may remain nominal, signal quality degrades. Recognizing this phenomenon helps avoid misinterpretation and prompts repositioning or warming of the extremity.
SpO₂ and Temperature: The Thermodynamic Connection
The Role of Body Temperature in Tissue Oxygen Demand
Temperature influences basal metabolic rate and oxygen consumption. Fever accelerates tissue oxygen demand, often causing subtle declines in SpO₂. Hypothermia, on the other hand, suppresses metabolism but also compromises peripheral perfusion—impacting sensor accuracy.
Peripheral Vasoconstriction and Signal Strength in Cold States
In cold environments or hypothermic states, vasoconstriction reduces blood flow to extremities, weakening the pleth signal. SpO₂ sensors may struggle to register accurate values. Combining temperature and SpO₂ data guides clinicians to distinguish between true hypoxia and technical artifact.
Febrile Patients and Changes in Metabolic Oxygen Consumption
In febrile patients, the body’s oxygen demands rise, and any pre-existing cardiopulmonary compromise becomes more apparent. Monitoring SpO₂ in the context of elevated temperature helps anticipate decompensation, especially in patients with chronic respiratory or cardiovascular conditions.
Real-Time Monitoring: The Synergy of Combined Parameters
Data Fusion for Early Warning Scores and Risk Stratification
Modern monitoring systems use integrated data to calculate Early Warning Scores (EWS) or Modified Early Warning Scores (MEWS). These algorithms assess changes across SpO₂, ECG, NIBP, and temperature to quantify patient risk. Data fusion creates a more sensitive and specific risk signal than any parameter in isolation.
How Smart Monitors Aggregate SpO₂, ECG, NIBP, and Temp into a Single Display
Multi-parameter monitors synchronize data streams into a unified interface. Waveforms, numeric trends, and alarms are contextualized across systems. This integration enables clinicians to grasp the whole clinical picture with a single glance, minimizing error and cognitive overload.
Alarm Management and Event Correlation in Multi-Parameter Systems
False alarms are a notorious issue in intensive care. Integrated systems reduce alarm fatigue by correlating events—e.g., only triggering a desaturation alarm if accompanied by bradycardia or hypotension. This contextual filtering enhances clinical response and reduces unnecessary disruptions.
Clinical Applications of Integrated Monitoring
Anesthesia and Surgery: Maintaining Stability Across All Vitals
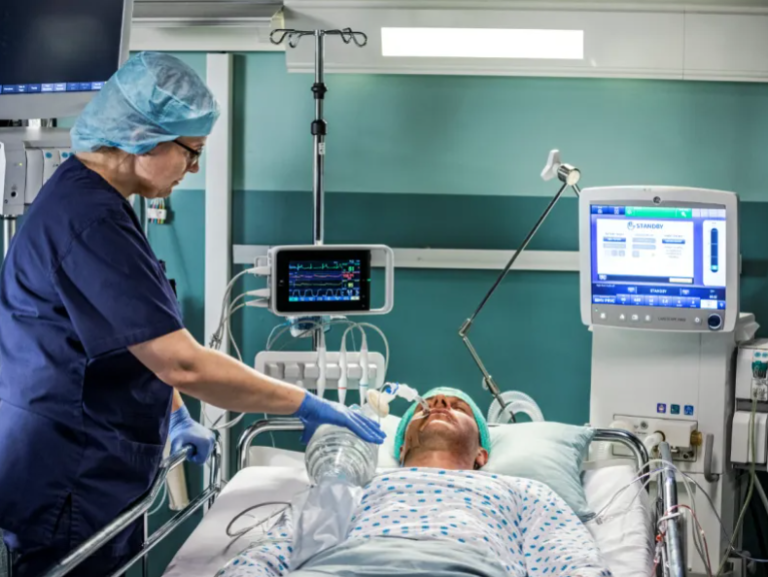
Intraoperative monitoring requires simultaneous tracking of SpO₂, ECG, NIBP, and temperature to ensure anesthesia depth, hemodynamic balance, and respiratory adequacy. Integrated monitoring helps anesthesiologists detect early signs of hypoxia, arrhythmia, or blood pressure instability, safeguarding patient outcomes.
ICU and Emergency Use: Rapid Decision-Making Based on Combined Metrics
Critically ill patients undergo rapid physiological shifts. The ability to analyze multiple vitals in concert enables ICU teams to react with precision—whether it’s initiating mechanical ventilation, titrating vasopressors, or administering antipyretics. Emergency teams likewise rely on multi-parameter dashboards for real-time triage.
Remote and Home Monitoring: Simplified Dashboards for Complex Data
For chronic disease management and post-discharge care, integrated portable monitors deliver essential insights with user-friendly dashboards. Home SpO₂ readings gain more meaning when viewed alongside heart rate and temperature, helping patients and caregivers detect early warning signs and avoid hospitalization.
Conclusion
Seeing the Bigger Picture: Why SpO₂ Alone Is Not Enough
While SpO₂ remains a cornerstone of respiratory monitoring, its value multiplies when viewed within the broader landscape of vital signs. Integrated monitoring transcends fragmented observation, offering a panoramic view of human physiology in motion. It is this layered insight that enhances early detection and improves clinical outcomes.
Moving Toward Predictive, Context-Aware Patient Monitoring Systems
As technology advances, we’re heading into an era of predictive, AI-enhanced monitoring—where SpO₂, ECG, NIBP, and temperature data will not only inform but forecast. These systems will recognize deteriorating trends before they become critical, transforming reactive care into proactive intervention. In the realm of patient safety, integration isn’t a luxury—it’s the new standard.
11.png)