A Comprehensive Exploration of Calibration Protocols, Technology, and Regulatory Standards
Introduction
The Vital Role of Calibration in SpO₂ Sensor Reliability
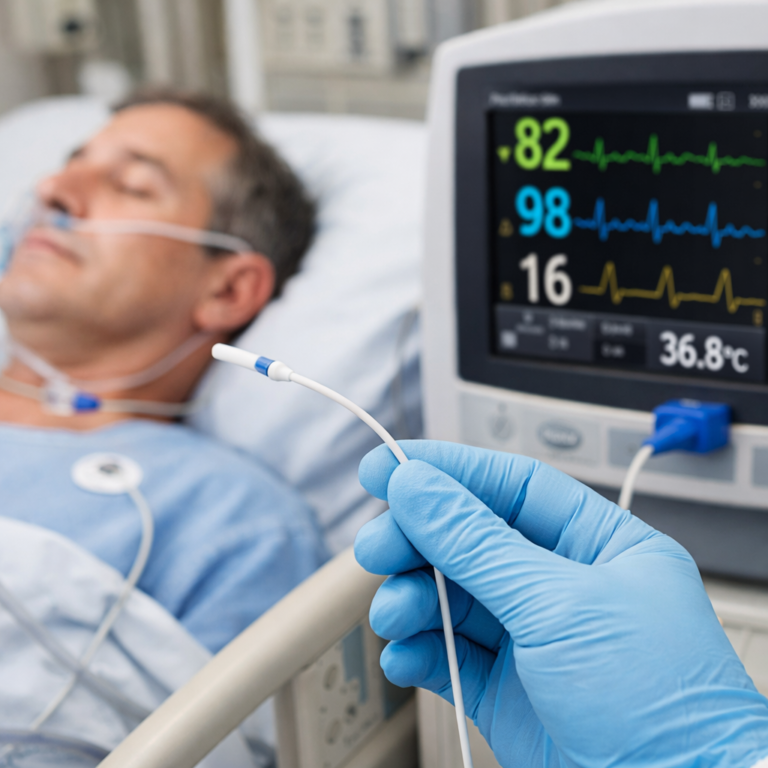
In clinical settings where every second matters, the reliability of an SpO₂ sensor can determine whether a patient receives timely intervention or experiences avoidable deterioration. Calibration is the invisible backbone behind the numbers displayed on patient monitors. Without it, the data is merely noise. Precision calibration ensures the sensor’s optical signals correspond accurately to real physiological conditions—no matter the patient, movement, or environmental variability.
Why Accuracy in Blood Oxygen Monitoring Can’t Be Left to Chance
Blood oxygen saturation is a critical parameter in diagnosing respiratory failure, titrating oxygen therapy, and monitoring anesthesia. Inaccurate SpO₂ readings can lead to missed hypoxemia, unnecessary escalations of care, or false alarms. That’s why clinical-grade sensors undergo rigorous, repeatable calibration processes—because accuracy isn’t a convenience in healthcare; it’s an imperative.
Fundamentals of SpO₂ Calibration
What Does Calibration Mean in the Context of SpO₂ Monitoring?
In SpO₂ monitoring, calibration is the process of aligning the sensor’s optical output and detection readings to known physiological reference values. This ensures that the sensor doesn’t just respond to changes in light—it responds meaningfully, producing clinically interpretable oxygen saturation data. Calibration bridges the gap between raw photoplethysmographic signals and actionable diagnostics.
Distinguishing Between Factory Calibration and Field Calibration
Most clinical SpO₂ sensors are factory-calibrated during production using advanced laboratory protocols. These calibrations are locked into the sensor’s firmware or signal processing algorithms. Field calibration, on the other hand, typically refers to functional verification or performance checks done in a healthcare facility. Unlike temperature probes or blood pressure cuffs, SpO₂ sensors rarely require recalibration in the field due to the stability of their embedded algorithms.
Clinical Calibration Models
Using Arterial Blood Gas (ABG) Measurements as a Calibration Reference
The gold standard for oxygen saturation is arterial blood gas analysis, specifically the SaO₂ value measured via co-oximetry. During calibration, SpO₂ readings are compared against ABG-derived SaO₂ levels under controlled physiological conditions. This benchmark ensures that the sensor’s output correlates closely with invasive laboratory methods, especially across critical saturation ranges.
The Role of Controlled Desaturation Studies in Human Volunteers
To develop accurate calibration curves, manufacturers conduct controlled desaturation studies involving healthy human subjects. In these highly supervised environments, oxygen levels are gradually reduced—within safe parameters—while ABG samples and SpO₂ readings are taken concurrently. These paired data points form the empirical basis for signal-to-saturation mapping.
Creating Population-Based Calibration Curves from Clinical Trials
Calibration is not one-size-fits-all. Differences in physiology, skin tone, age, and perfusion levels must be considered. Manufacturers often aggregate desaturation study data from diverse populations to build statistically robust calibration curves. These population-based models allow sensors to perform reliably across broad demographic and clinical scenarios.
Mathematical and Algorithmic Calibration
Ratio-of-Ratios: The Core Principle in SpO₂ Estimation
At the heart of SpO₂ computation is the “ratio-of-ratios” method. The sensor measures the absorption of red and infrared light at two wavelengths. By analyzing the ratio of pulsatile to non-pulsatile absorption at each wavelength, and then comparing those ratios, the system derives an estimated SpO₂ value. Calibration aligns these computed ratios with real-world saturation values from clinical studies.
Correction Factors for Skin Pigmentation, Thickness, and Motion
Human variability can introduce distortions. For example, melanin absorbs light differently, and tissue thickness can scatter optical signals. Sophisticated calibration includes compensation algorithms that adjust for these variabilities. Additionally, motion artifacts—common in conscious or pediatric patients—are algorithmically filtered without skewing the underlying saturation estimation.
Adaptive Algorithms for Signal Averaging and Real-Time Recalibration
Modern SpO₂ sensors incorporate adaptive averaging algorithms that respond to the stability of the signal. During stable conditions, averaging tightens to deliver faster readings; during movement or low perfusion, the system expands averaging windows and applies real-time recalibration to maintain accuracy. This dynamic adaptation is a product of rigorous pre-programmed calibration logic.
Sensor Recalibration: Myth or Necessity?
Why Most Clinical Sensors Are Factory-Calibrated for Life
Unlike analog devices, most SpO₂ sensors do not drift significantly over time. Their core light-emitting and detecting components are digitally programmed, with calibration parameters embedded in their architecture. Unless damaged or degraded, these sensors maintain their accuracy throughout their lifecycle without recalibration.
Scenarios That May Require Recalibration or Functional Verification
While full recalibration is rarely required, there are instances where verification becomes necessary. This includes after exposure to extreme sterilization methods, physical damage, or unexpected deviations in readings. In such cases, functional testing using simulators helps determine if recalibration—or outright replacement—is needed.
Differences Between Recalibration and Sensor Replacement
Recalibration involves adjusting algorithmic parameters or optical sensitivity—something rarely feasible outside the factory. In most cases, faulty or degraded sensors are replaced entirely. This ensures consistent performance without risking inaccurate modifications or unvalidated recalibration procedures in the field.
Simulators and Calibration Verification Tools
How Optical Simulators Are Used to Confirm Device Response
Optical simulators mimic tissue light absorption at specific saturation levels. When connected to a monitor, they produce synthetic signals corresponding to pre-set SpO₂ values. The monitor’s reading is then compared to the simulator’s standard, allowing technicians to verify calibration accuracy without requiring human test subjects.
Simulated Saturation Levels for Functional Testing
Simulators typically provide a range of saturation levels—e.g., 80%, 90%, 95%, 100%—to assess how the sensor and monitor respond across the clinical spectrum. These step tests can detect drift, lag, or algorithmic misalignment. More advanced simulators even replicate low perfusion or motion artifact scenarios for thorough performance evaluation.
Calibration Verification for OEM-Approved Compatible Sensors
Third-party or compatible sensors must also be verified for calibration integrity when paired with OEM monitors. Approved compatibility ensures the sensor’s output aligns with the host monitor’s algorithms. Calibration verification tools are critical to maintaining interoperability without compromising data accuracy.
Conclusion
Why Precision Calibration Is the Heartbeat of Reliable SpO₂ Monitoring
Behind every accurate oxygen saturation reading lies a tapestry of photonics, physiology, and data science—woven together by calibration. Precision calibration empowers clinicians to make confident decisions, ensuring that each SpO₂ percentage displayed reflects a reliable, life-critical truth. It’s not just about measuring light—it’s about measuring trust.
The Future of SpO₂ Sensor Accuracy in a Digitally Connected World
As sensors evolve alongside AI-driven diagnostics, remote monitoring, and wearable technology, calibration will become even more dynamic. We are entering an era of self-verifying, smart sensors capable of learning from use, adjusting in real time, and communicating seamlessly with digital ecosystems. But their core promise remains unchanged: accurate, trustworthy, and actionable readings at the heart of modern medicine.
11.png)